TRANSNASAL ENDOSCOPIC SURGERY - Dr. P. THULASI DAS
Fungal sinusitis appears to be on the rise. We either readily diagnose fungal Rhinosinusitis due to improved modalities such as CT scan & MRI scan and increased awareness on the part of the clinician or truly, there is an increase in the number of fungal sinusitis cases.
Fungal colonies on spoilt bread and on shoes during monsoon Precisely the same species of fungi are grown in the sinus cavities of humans
Fungus is so common in our environment, it is considered ubiquitous. When bread gets spoilt, the greenish colonies we notice are fungal colonies. The grayish colonies that grow on the leather shoes and moist walls during monsoon are fungal colonies. Fungus readily grows on decayed organic matter. Fungal spores may be floating freely in our atmosphere and we must be inhaling them. In some susceptible individuals, the fungus remains in the sinus cavity, and when an anaerobic environment is available, they multiply to form a fungal colony.
FUNGAL BALL
In normal individuals it forms a simple fungal colony called a fungal ball. Maxillary & Sphenoid sinuses are the most commonly affected sinuses. Simple, complete removal of the fungal colony is all that is required to cure this condition. Endoscopic Surgery plays a major role in the complete removal of fungal material. It is advisable to avoid external operations in these patients to prevent inoculation of fungus into the tissues.
ALLERGIC FUNGAL SINUSITIS
In atopic individual, in addition to forming colonies in the sinuses, the fungus produces systemic effects such as elevated IgE and positive skin tests. The ethmoid sinus is commonly affected and the inflammatory reaction to the fungus produces massive polyps and characteristic allergic mucin. Patients present with typical allergy like symptoms, nasal block, anosmia, rhinorrhea, sneezing and proptosis.
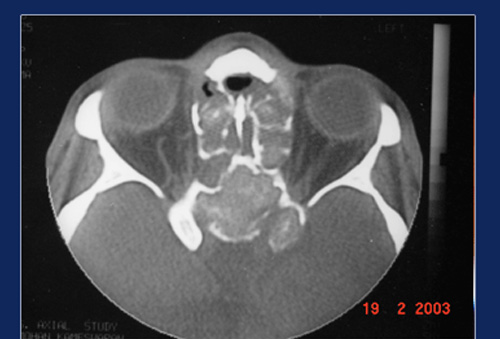
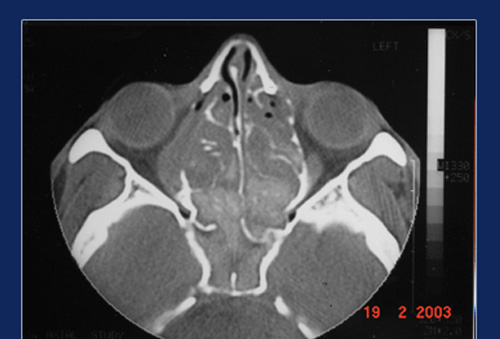
CT scan study of sinuses show typical hyper attentuation inside the sinus cavity called “Metal Dense” shadows. This is due to the fungus trapping heavy metals likes calcium & magnesium. MRI scan show hypointensity of the same areas on T1 – weighted images and signal void on T2 – weighted images.
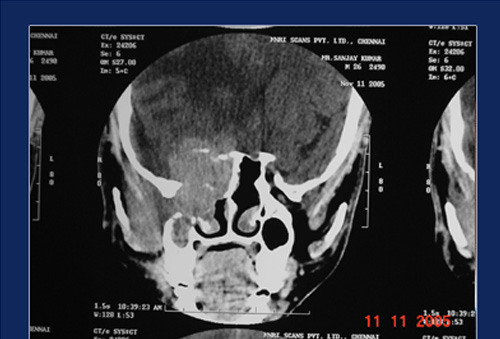
Expanded sinuses in allergic fungal sinusitis Hyperdense areas suggestive fungal colonies
Fungus shows remarkable ability to expand the sinus walls, so much so the lesions may protrude into the orbit or cranial cavity. Expansion of the ethmoids and frontal sinuses may produce proptosis ( bulging of the eyes). Expansion of sphenoid sinuses may produce loss of vision due to pressure on the optic nerve.
Endoscopic Surgical clearance of the fungal material and polyps with marsupialisation of all the sinuses for better ventilation and drainage followed by systemic steriods seem to control the disease. Allergic fungal sinusitis is notorious for recurrence. Minor procedures may be required periodically. The role of anti fungals are not established for this condition.
After having treated more than 500 cases of allergic fungal sinusitis and fungal balls in the last 15 years, we are of the opinion that Antifungals do not really help in allergic fungal sinusitis
CHRONIC INDOLENT OR GRANULOMATOUS FUNGAL DISEASE
Chronic indolent or granulamatous fungal disease affects apparently healthy individuals. Usually the disease affects the orbit and brain. Though the starting point may be in the sinus, once the fungus gains entry into the orbital fat or brain it spreads like wild fire. The body’s own defence mechanism puts up a fight and granulomas form. It is usually very thick scar tissue. Cutting instruments have to be used even to take a biopsy.
Destruction of tissue planes are typical and it makes en masse excision difficult
Small lesions respond well to anti fungal treatment. But large lesions involving the orbit and cranium are refractory to antifungal treatment. Surgical excision combined with longterm antifungal treatment helps in controlling the disease. Aspergillus is the commonest organism and hence it also called chronic indolent aspergillosis.
ACUTE MUCORMYCOSIS
Mucor is an opportunistic fungus present as a commensal in the throat and nose of normal individuals. In diabetics and immuno compromised individuals the mucor becomes pathological to produce an acute sinusitis with tissue destruction. Maxillary sinus is commonly affected, typically with whitish mucopus and bone destruction. The adjacent sinus walls are eroded and CT shows bone demineralisation and pathological fracture of sinus walls. The treatment is Endoscopic debridement and control of diabetes. Usually the sinus returns to normal even without antifungal treatment. Many sittings of debridement may be required and sometimes abscess formation may occur in the pterygopalatine or infra temporal fossae which has to be drained. On the whole, it carries good prognosis if treatment is started early.
Consult Us
-
Nasal Block
Nasal block only at night or both during day and night is cause for concern. Chronic nasal block has systemic effect.. read more
-
Repeated attacks of cold
Repeated attacks of cold once or twice a month or every 2 months is not normal. Almost everybody.. read more
-
Sneezing
Sneezing is a protective reflex. A few sneezes a day, in fact, are good, to clear the nasal cavity and the lungs.. read more
-
Watery drip from the nose
Watery drip from the nose can be due to allergic rhinitis, Vasomotor rhinitis or CSF rhinorrhoea.. read more
-
Anosmia
Anosmia is loss of smell sensation. Nasal polyps, chronic ethmoid sinusitis, chronic nasal obstruction all.. read more
-
Headache and Heaviness
Headache is the commonest symptom experienced by human beings. There are numerous causes.. read more
-
Hearing Loss
Among others, otosclerosis is a common cause for hard of hearing. It is a hereditary condition.. read more
-
Cleft lip nose
Most primary cleft lip and palate repairs are done by plastic surgeons. There are not many takers for secondary.. read more
-
Difficulty in breathing
Difficulty in breathing may be due to nasal block or narrowing of larynx or trachea. The narrowing of larynx.. read more